Willem Kolff was a young Dutch doctor working on his PhD and medical residency at Groningen University in 1940. He had traveled to The Hague for a family funeral when German planes bombed the barracks and began dropping leaflets warning of an invasion. He rushed to the hospital, and asked if they had a blood bank. The answer was no. Soon he was heading around the city with purchase orders and an armed escort to get everything he needed to start a blood drive.
Kolff had grown up in Leiden and followed his father, who ran a tuberculosis clinic, into medicine, getting his degree from the University of Leiden in 1938. At the time of his training, transfusions went directly from the donor to the patient. While in residency for his credential in internal medicine at Groningen, Kolff began to develop methods to store blood for later use, so he was prepared to start what was continental Europe’s first blood bank.
The German invasion had quickly overtaken The Netherlands, and Nazi sympathizers were installed in government and hospital administration. Looking for a place to work, Kolff found a position in a small hospital in Kampen. There he took up a problem of blood chemistry that plagued him, after he attended a young man who was suffering from kidney failure, and died a horrible death. Yet Kolff knew that the amount of urea in the blood that led to his death was in total a very small amount. He wanted to find a solution to clean the blood when the kidneys couldn’t, and a mentor at Groningen had given him a clue.
Research in animals showed that cellophane, commonly used then in sausage casings, could be used as a filter for solutions of small chemicals. Kolff experimented with blood and sausage casings, and these experiments led to the development of the first ‘artificial kidney,’ which led to modern dialysis. Because of wartime shortages and Nazi supervision, his research and development had to stay secret, and Kolff used repurposed materials.
The first ‘artificial kidney’ was made from juice cans, sausage casings, and parts from an old washing machine. Gravity was used to force the blood through a filter, instead of a pump, and the tubes were rotated around a drum into a dialysis solution. While working at the hospital, Kolff worked with the Resistance, and ultimately helped hide around 800 people who the Nazis sought for deportation to work camps.
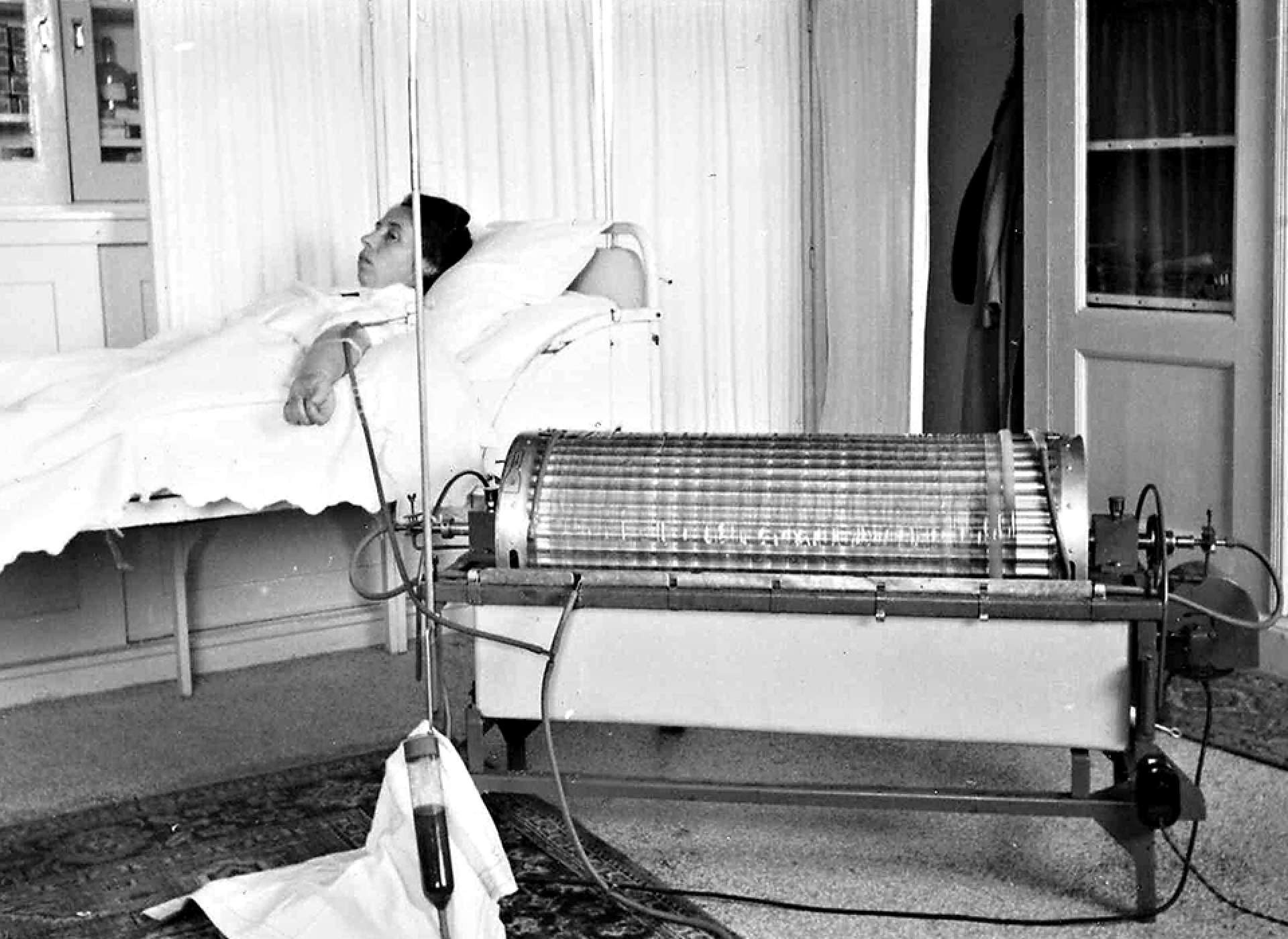
A demonstration, with a nurse acting as patient, of how the dialysis machine would work. Courtesy of the Marriott Library at the University of Utah.
During the war, Kolff tested his device on patients who came in with kidney failure, and were dying. They had no other hope for a treatment. 15 patients came in, and despite some minor successes, they all died. As Kolff tested different dialysis solutions, and treatments of the blood with anticoagulant, they lived longer. A 16th patient came in, a woman in the end stages of renal failure who was comatose. She was a known Nazi collaborator who would become a prisoner after the Liberation. Kolff treated her without prejudice. Maria Schafstad became the first successful patient treated with the artificial kidney in 1945.

The dialysis machines hidden from the view of occupying German authorities in the garden of the hospital at Kampen. Courtesy of the Marriott Library at the University of Utah.
With the war ending, Kolff returned to Groningen to complete his PhD, using the research on the ‘artificial kidney,’ or hemo-dialysis in his dissertation. In 1947 he shipped one of the devices to Mt. Sinai Hospital in New York, and began collaborations with researchers there to improve the device. In 1950 he emigrated to the United States and took a position at the Cleveland Clinic, where he spent six years researching, learning English, retaking his medical exams in English, and becoming a US citizen.
Kolff’s research at that time was on a machine to oxygenate blood. He had a new goal: to develop an artificial heart. He moved to the University of Utah in 1967, and became leader of a project to develop an artificial heart and mentor to Dr. Robert Jarvik who is credited with developing the first permanent artificial heart. Willem Kolff died in 2009.
“Whenever I see a problem,” Willem Kolff once said, “I try to reduce it to simple terms. If the problem is very complicated I look at whether or not there is a simple component to it. And if the simple component is an important part, I take that first.”
Rob Wallace
Rob runs teacher workshops and develops curriculum, including Real World Science, funded by The Northrop Grumman Foundation.
Cite this article:
MLA Citation:
APA Citation:
Chicago Style Citation:







![Max Fuchs, New York City cantor, sings as Rabbi Sydney [sic] Lefkowitz, Richmond, VA, conducts the first Jewish services from Germany.](/sites/default/files/styles/max_650x650/public/2025-10/image1.jpg)