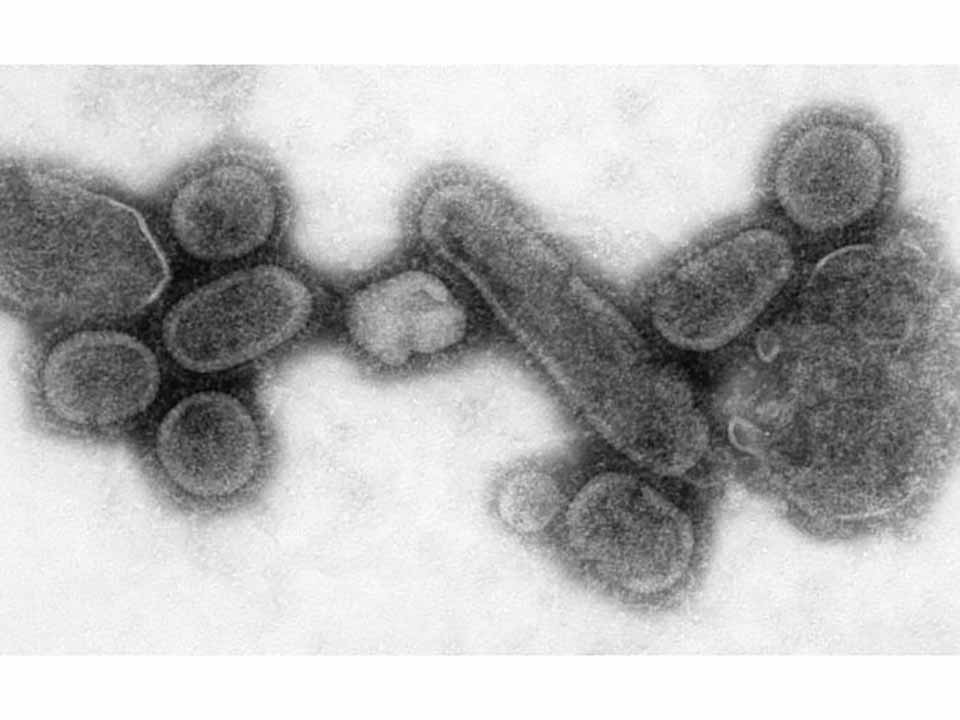
In 1918 a pandemic influenza killed an estimated 50 million people across the globe, or 3 percent of the world’s population. This estimate is conservative and likely low, as worldwide systems to track civilian deaths were not in place. The first cases presented in January of 1918, and the last were in 1920. Most deaths occurred in the fall of 1918, with another outbreak in the spring of 1919. This was not the first time a wave of influenza had passed across the world, but it was by far the worst.
This pandemic has been referred to as the Spanish flu. That name is misleading. Spain was neutral in World War I, so the Spanish press was left free to publish information about the spread of the disease, and thus the initial news about the pandemic came from Spanish sources. There are many hypotheses about where this strain of influenza originated, but none of them center on Spain. It might have begun in the Midwest United States, where there were widespread contemporaneous cases of influenza in pig livestock. Wherever it began, its impact was worldwide, and the transport of large numbers of servicemen certainly exacerbated the situation.
Much of Europe was decimated by World War I, and the direct impacts of that destruction, in economic, environmental, demographic, and political terms, left the continent in an unstable state. Coming at the end of World War I, the 1918 flu pandemic was a great contributor to instability not only in Europe, but around the world. The month of peak mortality in the pandemic was November 1918—the same month that the war ended. The US Navy and Army estimated that 40 percent and 36 percent of their servicemen had been affected. The descriptions of this pandemic disease are gripping, and the pattern of who was struck was different than in previous outbreaks. I will suggest further reading if readers want to learn more about the 1918 pandemic at the end of this article. What I want to focus on here is the response to the pandemic, and how it influenced the next century of medical innovations—including those of the World War II era.
At the time of the 1918 pandemic, medical experts did not know its causes, and at the beginning there were no effective treatments. By the end of the pandemic, treatment by transfusion of blood from a survivor was known to be effective. But transfusion methods were rudimentary, performed directly from donor to patient, and blood typing and matching was in its infancy.
Scientists thought that influenza was caused by a bacterium they called Baccilus influenzae (now known as Hemophilus influenzae.) They could isolate and see many types of bacteria under a microscope. They also knew that there were disease agents smaller than bacteria that they could filter out of a mixture. Not being able to view these very small agents, there was a debate about whether they were chemicals or very small organisms. However, vaccines against these very small agents, which they called viruses, had already been developed going back to the smallpox vaccine in late eighteenth century.

Richard Shope, who demonstrated that the 1918 pandemic was caused by a virus, and connected the human and swine flu viruses. Courtesy of the National Library of Medicine.
In the decades following the pandemic, scientists did not forget the danger of influenza, and worked to develop a better understanding of the disease. In 1931, Richard Shope studied pigs carrying swine flu, and applied procedures used in earlier decades to identify the causes of yellow fever and other diseases. He found that the presence of H. influenza made swine flu worse, but did not cause it. In 1936, Shope showed that people living and working on the pig farms had antibodies to the swine flu, showing that the human and swine disease were closely related. Contemporary researchers developed techniques to view such small particles using electron microscopes, and chemically identified them as being made up primarily of protein and ribonucleic acids.
In 1931, a huge innovation was made at Vanderbilt University. Researchers there found ways to grow the influenza virus in fertile chicken eggs. This meant that they no longer had to get them from sick people or animals. Growing viruses and comparing immunological responses of lab animals, scientists identified two types of flu viruses, naming them A and B. The 1918 pandemic virus was a Type A virus. Today we know that Type A viruses infect both humans and some other animals, and are more dangerous. Type B viruses are in humans only.
With the ability to grow quantities of the viruses, and to identify their characteristics, researchers in the late 1930s began working on a vaccine. In 1937, with pressure to prepare for another war growing, British researchers tested a vaccine on soldiers, and in 1938 the US Army began tests of vaccines with a research team that included Jonas Salk. The first mass use of an influenza vaccine for soldiers in the United States came in 1944, and for civilians, in 1945. During the research for this vaccine, it was discovered that immunity against one type of virus does not give immunity against the other. So the vaccine contained a mixture of both types—a precedent still followed today.
The search for the virus, and a vaccine to prevent the influenza, led to a number of other discoveries. It created tools for the development of other vaccines. Today we still use fertile eggs to grow viruses. It also led to our understanding of the nature of genes and the chemicals that encode them. Oswald Avery, a researcher at the Rockefeller Institute, led the team that discovered in 1944 that deoxyribonucleic acid (DNA) held the genetic code. Their research used tools developed in identifying the parts and types of viruses, and used a bacteria that causes pneumonia. Avery’s work built on the very important work of Frederick Griffiths, work that Avery initially set out to disprove. Tragically, Griffiths, who was a British scientist, died in the Blitz in 1941.
This story shows many of the hallmarks that distinguish advancements in the history of scientific innovation: collaboration of researchers across institutions and nations, the serendipitous discovery of phenomena and tools that become keys to answering other questions, and the creativity that researchers use in the face of necessity. It also shows that big events in history are not separate—the events of World War II were much influenced by those in World War I.
The events of today are the fruit of past decisions, and our options for responses to them can be found in those of our predecessors.
To read more about the 1918 Influenza Pandemic, I suggest The Great Influenza by John Barry, and for more on research on the virus and it’s scientific legacy I suggest Flu: The Story of the Great Influenza Pandemic of 1918 and the Search for the Virus That Caused It by Gina Kolata.
Rob Wallace
Rob runs teacher workshops and develops curriculum, including Real World Science, funded by The Northrop Grumman Foundation.
Cite this article:
MLA Citation:
APA Citation:
Chicago Style Citation: